Your clinical results are excellent. Your before-and-after gallery is impressive. Your pricing is competitive. And yet patients aren’t coming back — and they’re not sending referrals either.
More often than not, the problem isn’t the treatment. It’s everything around it.
In aesthetic medicine, patient experience is your product. Not just the Botox, the filler, or the laser treatment — the entire arc from first inquiry to follow-up call. Every touchpoint your staff controls either builds patient loyalty or erodes it. And because most practices put their training dollars into clinical skills, the experience side often gets neglected.
This guide covers what a real patient experience training program looks like — the frameworks, the scripts, the culture shifts, and the metrics that actually matter.
Why Patient Experience Is Your Most Powerful Marketing Tool
Before diving into the training itself, it helps to understand the business case.
According to research from Bain & Company, increasing patient retention by just 5% can boost revenue by 25–95%. In aesthetic practices, where procedures are high-ticket and repeat visits are common, that math is significant. A single loyal patient who comes in for quarterly treatments and refers two friends per year is worth dramatically more than a one-time visitor — even if that one-time visitor books a more expensive procedure.
Here’s what drives loyalty in aesthetics:
- Trust — patients put their face and body in your hands; every interaction either reinforces or undermines that trust
- Feeling heard — aesthetic concerns are personal; patients who feel dismissed don’t return
- Consistency — a great experience one visit followed by a mediocre one creates doubt
- Follow-through — practices that check in post-procedure show they care about outcomes, not just bookings
None of these are clinical skills. All of them are trainable.
The 5 Stages of the Patient Journey Your Staff Must Own
Every patient interaction maps to one of five stages. Training should address each one explicitly.
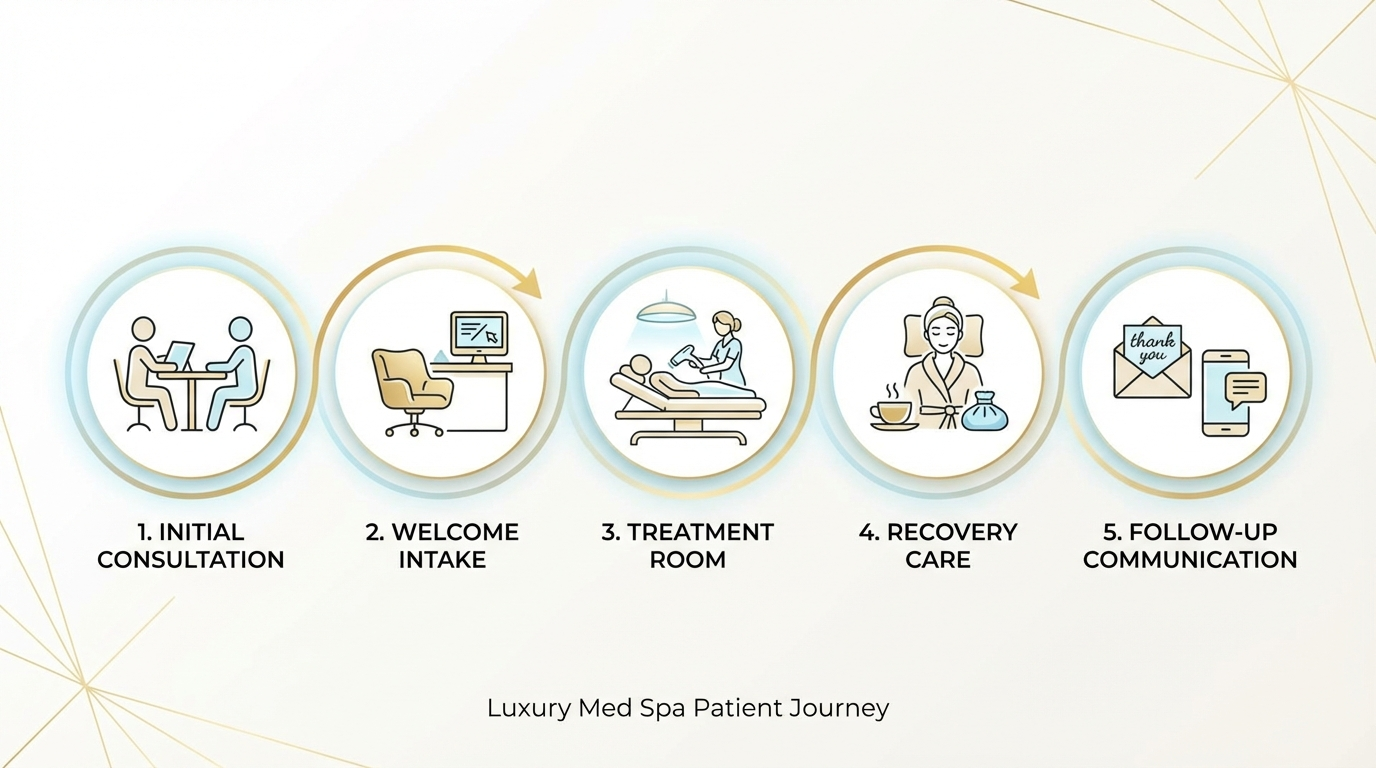
Stage 1: First Contact (Phone, Chat, or Online Inquiry)
The first response sets the tone. Practices that reply to inquiries within five minutes are 100 times more likely to convert than those that wait 30 minutes, according to the Harvard Business Review. Staff manning phones, chat, or intake forms need to be trained on:
- Warm, professional tone — not overly clinical, not overly casual
- Active listening — repeating back what the patient has said (“So you’re interested in addressing some volume loss in your cheeks — is that right?”)
- Setting expectations — what happens next, how long the process takes, what to prepare
- No dismissiveness — questions about pricing, recovery, or “Are your results natural-looking?” are not annoying; they’re buying signals
Stage 2: Intake and Check-In
The waiting room experience and intake process often feel transactional. Training should make them feel personal. Staff should:
- Greet patients by name when they arrive
- Offer beverages or comfort items without waiting to be asked
- Confirm the consultation purpose and any prior notes (“I see you’ve been thinking about ____ — Dr. [Name] is excited to talk through your options”)
- Never leave a patient waiting without explanation — if there’s a delay, acknowledge it proactively
Stage 3: The Consultation and Treatment
Providers typically receive the most training here, but front-of-house and treatment room assistants need attention too. For non-providers, training should cover:
- Room preparation — a pristine, organized treatment room signals professionalism
- Patient modesty and dignity — never leaving patients unnecessarily exposed, always narrating what’s happening
- Emotional attunement — recognizing when a patient is nervous and responding appropriately (“It’s totally normal to feel a little anxious before the first time — most patients are surprised by how quick and comfortable it is”)
Stage 4: Post-Treatment Care and Checkout
The experience often ends too abruptly. Checkout is a missed opportunity for connection and retention. Train staff to:
- Review aftercare instructions verbally, not just hand over a sheet
- Schedule the next appointment before the patient leaves (“When would you like to come back for your touch-up? We can lock in the same time slot right now”)
- Acknowledge the commitment the patient made (“This is going to look amazing — give it 2 weeks and you’ll love it”)
- Ask for feedback before the patient walks out, not just via email
Stage 5: Follow-Up
This is where most practices fall short — and where loyalty is actually built. Train your team (or implement automation) to:
- Send a personal follow-up 48–72 hours post-treatment: “How are you feeling? Any questions about your aftercare?”
- Check in at 2 weeks to ask about results
- Reach out before their expected return window expires (“It’s been about 3 months since your last appointment — would you like to book your follow-up?”)
Our guide on automating appointment reminders covers the tools that make this follow-up touchpoint scalable across your full patient base.
What a Patient Experience Training Program Actually Looks Like
Most practices either train on the fly (new hire shadows a senior employee for two days and is set loose) or invest in one-time workshops that don’t stick. Neither approach works.
A real training program has structure, repetition, and accountability. Here’s what it should include:
Module 1: Brand Voice and Patient Communication Standards
Every staff member needs to know how your practice sounds — in writing and in person. This means defining:
- Tone descriptors: Are you warm and nurturing? Confident and clinical? Approachable and expert?
- Phrases to use and avoid: “Let me get that taken care of for you” vs. “That’s not my department.” “I completely understand your concern” vs. “We get that question a lot.”
- How to handle complaints: The LARA framework (Listen, Acknowledge, Respond, Act) is a simple tool for staff who don’t know how to handle an upset patient
Module 2: Consultation Support Skills
Front-desk and patient coordinators need to understand the procedures you offer — not at a clinical level, but at a conversational one. They should be able to:
- Describe what a procedure feels like and what recovery involves
- Answer common concerns without overpromising
- Recognize when a question needs to be escalated to a provider
Role-playing is essential here. Set up 15-minute mock consultations during team meetings. Have staff practice handling the most common objections: “Is it safe?” “Will I look natural?” “How long does it last?” “What if I don’t like the result?”
Module 3: HIPAA and Privacy Best Practices
This isn’t just a compliance requirement — it’s a trust signal. Training your staff on HIPAA is also training them to communicate in ways that reinforce patient confidence. Key areas:
- Never discussing patient details in waiting rooms or common areas
- How to handle requests for records or before/after photos
- Digital communication standards (what can be texted, what can’t, using HIPAA-compliant platforms)
Our HIPAA-compliant marketing guide covers the technology side of compliance for aesthetic practices.
Module 4: Handling Difficult Situations
Unhappy patients will happen. A staff member who handles a complaint poorly can cost you three five-star reviews’ worth of reputation. Train on:
- Staying calm and non-defensive when a patient is unhappy
- Never making promises that exceed the provider’s authority
- The right way to escalate (and who handles what)
- How to document complaints properly

Scripts Your Team Can Use Starting Tomorrow
Giving staff specific language removes ambiguity and builds consistency. Here are five ready-to-use scripts:
When a new patient calls:
“Thank you for reaching out to [Practice Name] — I’m [Name] and I’d love to help you. Can I ask what brought you to us today?”
When a patient asks about pricing before consultation:
“Great question — pricing is personalized based on your goals and what we recommend for your specific concerns. We’ll go over all of that in detail during your consultation so there are no surprises. Would you like to set that up?”
When a patient expresses nervousness:
“I completely understand — it’s totally normal to have some nerves, especially before your first procedure. Most patients actually tell us they were surprised by how comfortable it was. Dr. [Name] will walk you through everything step by step.”
Post-treatment follow-up call:
“Hi [Name], this is [Staff Name] from [Practice Name]. I’m just calling to check in and see how you’re feeling after your treatment. Do you have any questions about your aftercare, or anything I can help with?”
When a patient hasn’t booked in a while:
“Hi [Name], I wanted to reach out because it’s been a little while since we’ve seen you, and we wanted to make sure you’re happy with your results. We’d love to have you back in for a touch-up whenever you’re ready — I can hold your preferred time if that’s helpful.”
Building a Culture of Excellence (Not Just a One-Time Training)
Training is a start. Culture is what makes it stick.
Practices with consistently outstanding patient experiences share a few cultural traits:
Leadership models the standard. Providers who greet every patient warmly, who say thank you to staff in front of patients, who never dismiss concerns — they set the tone for the whole team.
Patient experience is a team KPI. If you’re measuring clinical outcomes but not patient satisfaction, you’re measuring half the business. Tie bonuses or recognition to Google review scores, referral rates, or post-visit survey results.
Debrief after difficult interactions. When a patient complaint comes in, don’t sweep it under the rug — treat it as training data. What could have been done differently? What script would help next time?
Celebrate wins publicly. When a patient leaves a glowing review mentioning a specific staff member by name, announce it at the next team meeting. Public recognition is a powerful reinforcer.
Our guide on patient review management for aesthetic practices covers how to systematize collecting and leveraging patient feedback.
Measuring Patient Experience: The Metrics That Matter
You can’t improve what you don’t measure. These are the indicators that tell you whether your patient experience training is working:
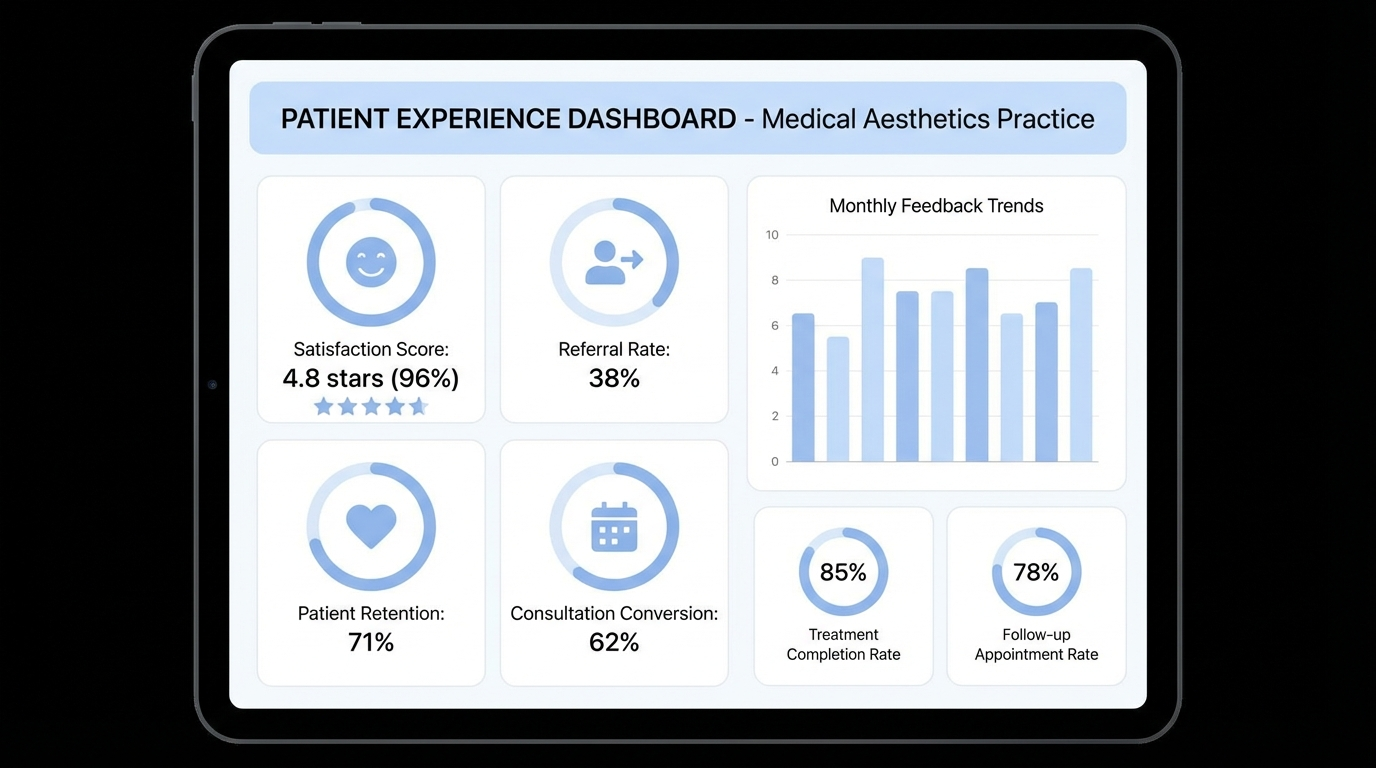
Net Promoter Score (NPS): “On a scale of 0–10, how likely are you to recommend us to a friend?” Anything above 50 is strong; above 70 is world-class. Survey every patient post-visit.
Return patient rate: What percentage of patients who complete a treatment come back for another within 12 months? Track this monthly. If it’s below 40%, experience may be a factor.
Referral rate: Ask every new patient “How did you hear about us?” If fewer than 20–30% of new patients come from referrals, you’re leaving loyalty-driven growth on the table.
Review score and velocity: Track your Google Business Profile average rating, but also track the number of new reviews per month. A declining review velocity often signals an experience issue before it shows up in ratings.
Consultation conversion rate: What percentage of consultations lead to a booked procedure? If this rate is declining without a pricing change, experience and communication are likely culprits.
For a deeper look at how to track and act on these numbers, our Google Analytics 4 guide for small businesses covers the tracking infrastructure that applies to aesthetic practices as well.
Getting Started: The 30-Day Training Plan
You don’t need to overhaul everything at once. Here’s a realistic first 30 days:
Week 1: Audit
- Mystery shop your own practice: call as a new patient, walk through the intake, pay attention to every touchpoint
- Survey your team: what do they feel confident about? Where do they feel undertrained?
Week 2: Prioritize
- Identify your top 3 experience gaps based on the audit
- Create or refine scripts for first contact, complaint handling, and post-treatment follow-up
Week 3: Train
- Run a 90-minute training session: present the patient journey framework, introduce the scripts, run role-plays
- Assign each team member one experience metric they personally own
Week 4: Measure and Iterate
- Send a one-question post-visit survey to the last 30 patients
- Review the results as a team and identify one process to improve immediately
Patient experience in aesthetics isn’t a soft skill — it’s a growth lever. The practices that understand this are the ones generating word-of-mouth referrals that no paid ad budget can replicate.
Ready to build a practice where patients become advocates? Talk to our team at Monsoft Solutions — we help aesthetic practices implement the systems, automation, and training frameworks that turn great clinical results into great businesses.
Related Reading:
- How to Automate Patient Appointment Reminders
- HIPAA-Compliant Marketing for Aesthetic Practices
- Patient Review Management for Aesthetic Practices
- Consultation Booking Optimization Guide
Frequently Asked Questions
How long does it take to see results from staff experience training?
Most practices notice measurable changes — higher post-visit survey scores, more verbal compliments, and fewer complaints — within 30 to 60 days of consistent training and reinforcement. Referral rates and return patient rates typically reflect changes over a longer period of 3 to 6 months.
Should patient experience training be different for front desk vs. clinical staff?
Yes. Front desk and patient coordinators need to focus on communication, intake, and complaint handling. Clinical assistants and treatment room staff need additional emphasis on patient dignity, emotional attunement during procedures, and aftercare education. Both groups need grounding in your brand voice and HIPAA basics.
What’s the most common mistake aesthetic practices make in patient experience?
The most common gap is abandoning the patient after checkout. Most practices invest in the consultation and treatment but have no systematic follow-up process. Patients who feel forgotten don’t return — and they definitely don’t refer. A simple 48-hour check-in text can make a significant difference in retention and loyalty.
How do you handle a patient who is unhappy with their results?
Train staff to listen without defensiveness, acknowledge the patient’s feelings, and immediately involve the provider or practice manager. Never dismiss concerns or make unauthorized offers. Document the interaction, follow up personally, and use the experience to refine your consent and expectation-setting process. A well-handled complaint can actually strengthen patient trust.
How often should patient experience training be refreshed?
New hires should receive a full onboarding training in their first week. For the full team, quarterly refreshers — tied to feedback data and any new service offerings — keep standards high. Annual deep-dives allow you to reset norms and address any culture drift that accumulates over time.
